While most breast cancers are sporadic, meaning there’s no genetic predisposition (i.e. gene variant inherited from one or both of your parents that increases your risk of breast cancer) that caused the cancer, around 5-10% of breast cancers are thought to be familial. Knowledge is power, and knowing if you have a genetic risk for breast cancer can empower you to take charge of your health by surveillance and managing your risk.

How do inherited gene variants increase a person’s risk for breast cancer? Everyone has two copies of genes that we inherit from our parents. These genes have many different variants in the human population, and some specific gene variants are associated with increased risk of breast cancer. For example, inherited mutations in BRCA genes that make the gene product non-functional (i.e. no longer able to repair damage to DNA) increase the risk for breast and other cancers because the loss-of-function allows other mutations to build up in affected cells, which can eventually transform them into cancer cells. If you carry BRCA variants associated with cancer, you may be at greater risk and you can also pass these risk genes to your children.
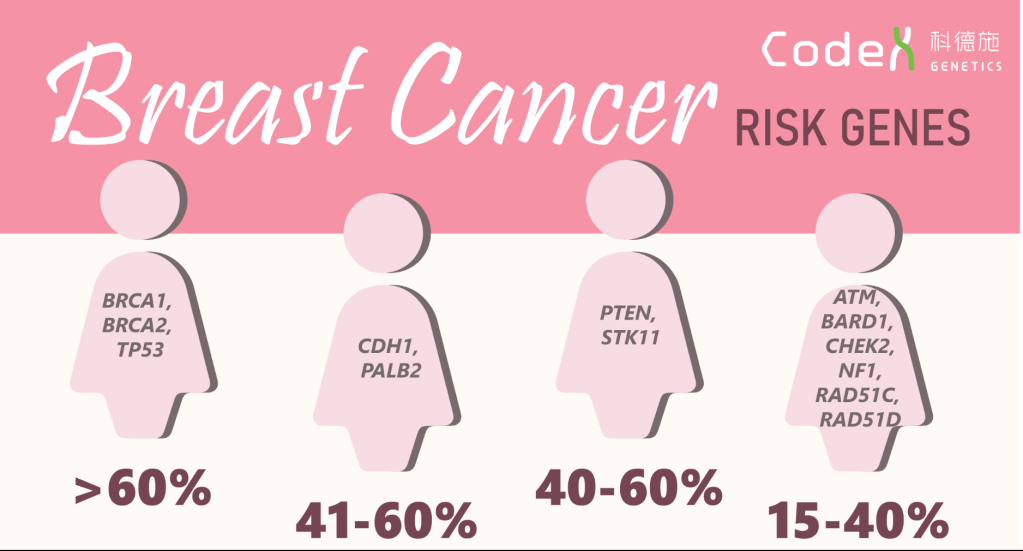
In addition to BRCA1 and 2 genes, other inherited gene variants have been identified that are associated with increased risk for breast cancer, as shown in the graphic below. Some of these genes, like TP53, PTEN, STK11, CHEK2, NF1, produce proteins that are also involved in regulating cell growth, so non-functional variants cannot put the breaks on cell growth and can cause cancer cells to grow uncontrollably. The PALB2, BARD1, ATM, and RAD51D gene products work like BRCA gene products to repair DNA damage, so loss of function increases the chance of accumulating mutations in cells, which can lead to cancer. The RAD51C gene product is involved in stopping cells with DNA damage from growing, so loss of function allows cells with mutations to divide and accumulate more mutations, which can lead to cancer.
Should you get genetic counseling and genetic testing? That’s a personal decision, but here are some recommendations from the CDC that might help you make your decision:
A strong family history of breast and ovarian cancer,
A moderate family health history of breast and ovarian cancer and are of Ashkenazi Jewish or Eastern European ancestry.
A personal history of breast cancer and meet certain criteria (related to age of diagnosis, type of cancer, presence of certain other cancers or cancer in both breasts, ancestry, and family health history).
A personal history of ovarian, fallopian tube, or primary peritoneal cancer.
A known BRCA1, BRCA2, or other inherited mutation in your family.
Knowing your risk can help you and your healthcare providers make decisions about surveillance and possible interventions. Take care of yourself, and if you can, find out about your family history of breast cancer.